Blog
Identify the ‘red flags’: reducing fraud and corruption during Covid-19 (Part 1 of 3)

Amid the pandemic U4, with the support of Norad, conducted media analysis and in-depth research on identifying corruption risks and real cases of Covid-19-related corruption worldwide. This work is part of a larger movement towards mainstreaming anti-corruption in the health sector, spearheaded by the Global Network on Anti-corruption, Transparency, and Accountability (GNACTA).
This blog is the first of a three-part series that identifies several corruption risks and their drivers at every level of a health emergency response. It also discusses how governments, businesses, health personnel, and citizens in general may be involved in the response. The series offers a practical guide to help those involved in implementing responses to better deal with the ongoing Covid situation, as well as future emergencies.
Corruption in health: a deadly business
To date, the WHO has issued four editions of its Covid-19 Strategic Preparedness and Response Plan (SPRP) – a package focused on 10 pillars to guide the coordinated action of health stakeholders at national, regional and global levels. Our research highlights how corrupt actors can co-opt each of these pillars, draining health budgets and reducing the effectiveness of health responses. We focus on the ‘red flags’ that can alert us to corruption risks; and how to mitigate them.
Table 1. The World Health Organization’s 10 emergency ‘response pillars’
|
Pillar number |
Description |
|
Pillar 1 |
Coordination, planning, financing, and monitoring |
|
Pillar 2 |
Risk communication, community engagement, and infodemic management |
|
Pillar 3 |
Surveillance, epidemiological investigation, contact tracing, and adjustment of public health and social measures |
|
Pillar 4 |
Points of entry, international travel and transport, and mass gatherings |
|
Pillar 5 |
Laboratories and diagnostics |
|
Pillar 6 |
Infection prevention and control, and protection of the health workforce |
|
Pillar 7 |
Case management, clinical operations, and therapeutics |
|
Pillar 8 |
Operational support, logistics and supply chains |
|
Pillar 9 |
Maintaining essential health services |
|
Pillar 10 |
Vaccination |
In this blog series, we will take a deep dive into Pillar 1 (blog 2) and Pillar 8 (blog 3). These pillars are important because of their cross-cutting nature, which means they can have cascading effects. If we identify and address a corruption risk with a high likelihood of occurring in a specific pillar of the emergency response (eg, coordination), this will help us make progress on mitigating corruption risks in all the other pillars mentioned above.
‘Red flags’ for corruption risks
‘Red flags’ are warning signs that efforts within a pandemic response may be vulnerable to fraud or corruption. These flags could refer to problems with a policy, institution, system, process, person, decision, supplier, contract, or any element along the response chain. The research, as published in bi-monthly newsletters and a final Issue on the U4 website during 2021 and 2022, uses media examples to draw out several red flags within each pillar – over 100 in total.
These red flags are key reference points for planners, programme managers, the public, and those tasked with oversight and ensuring health outcomes. They can be used as a checklist to spot potential fraud or corruption risks, and design mitigation strategies accordingly.
Figure 1, below, shows the dynamic nature of corruption risks between the pillars.
Figure 1. Examples of how the activities of Pillar 1 could open the way for risks to emerge in other pillars
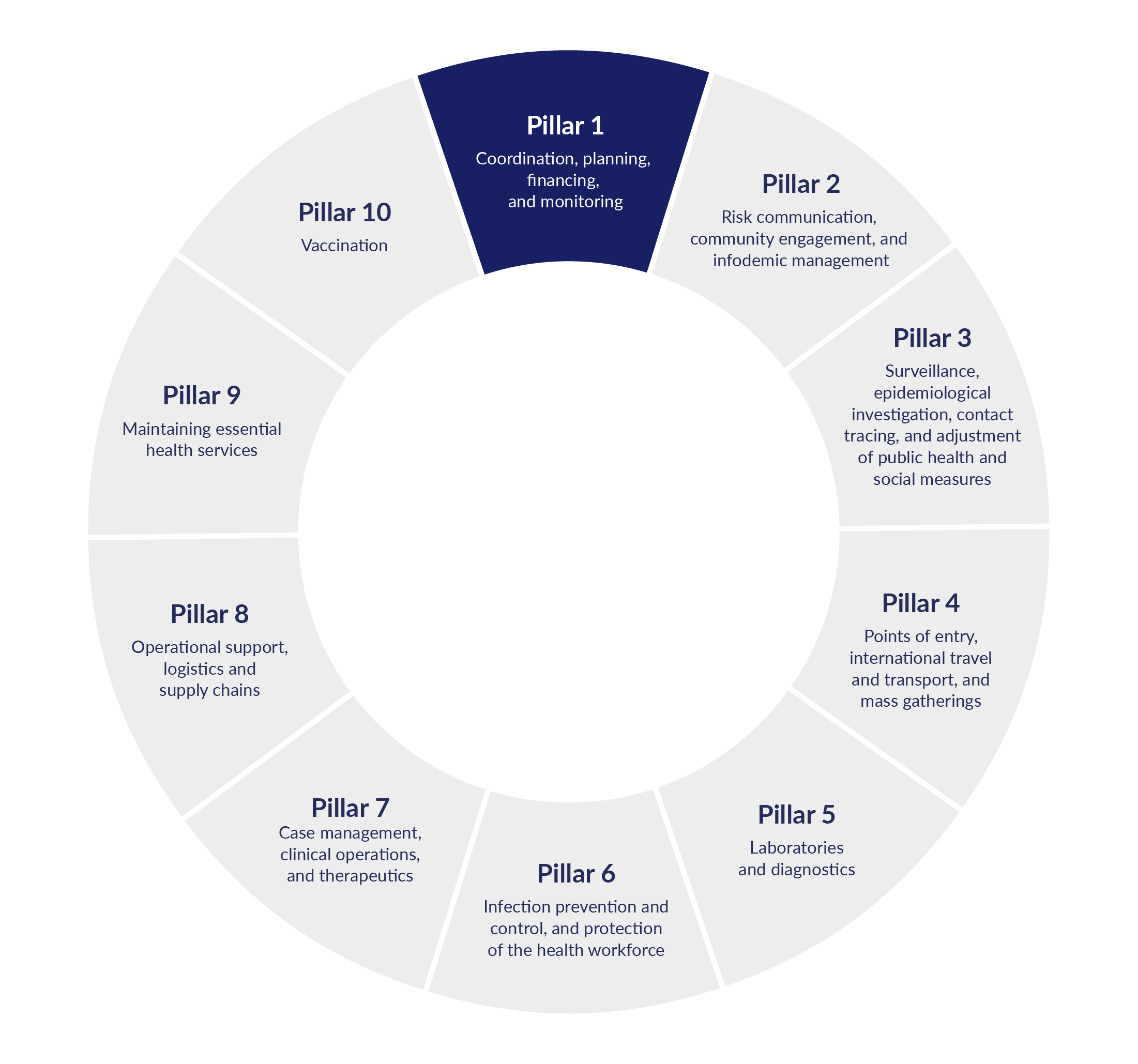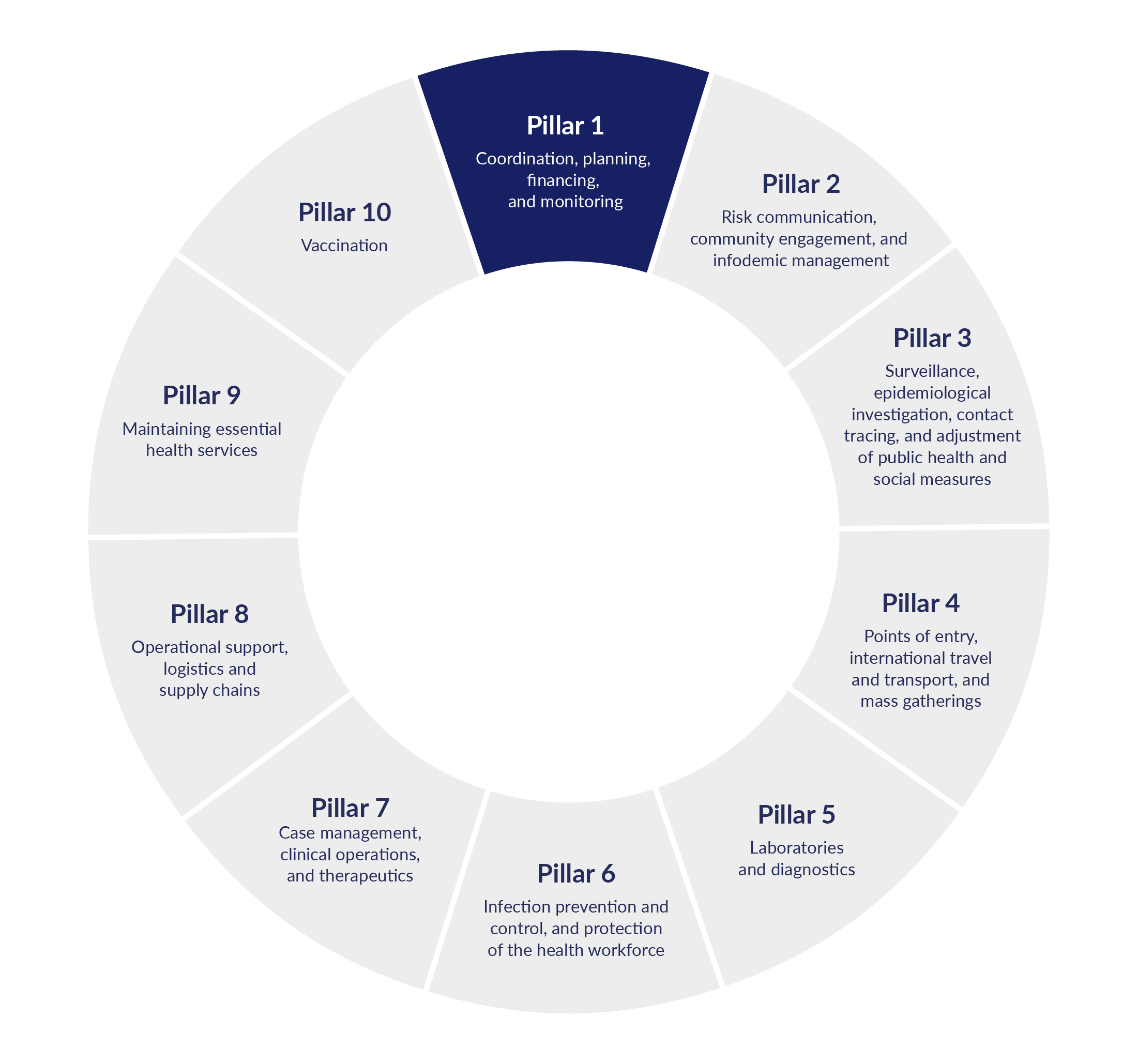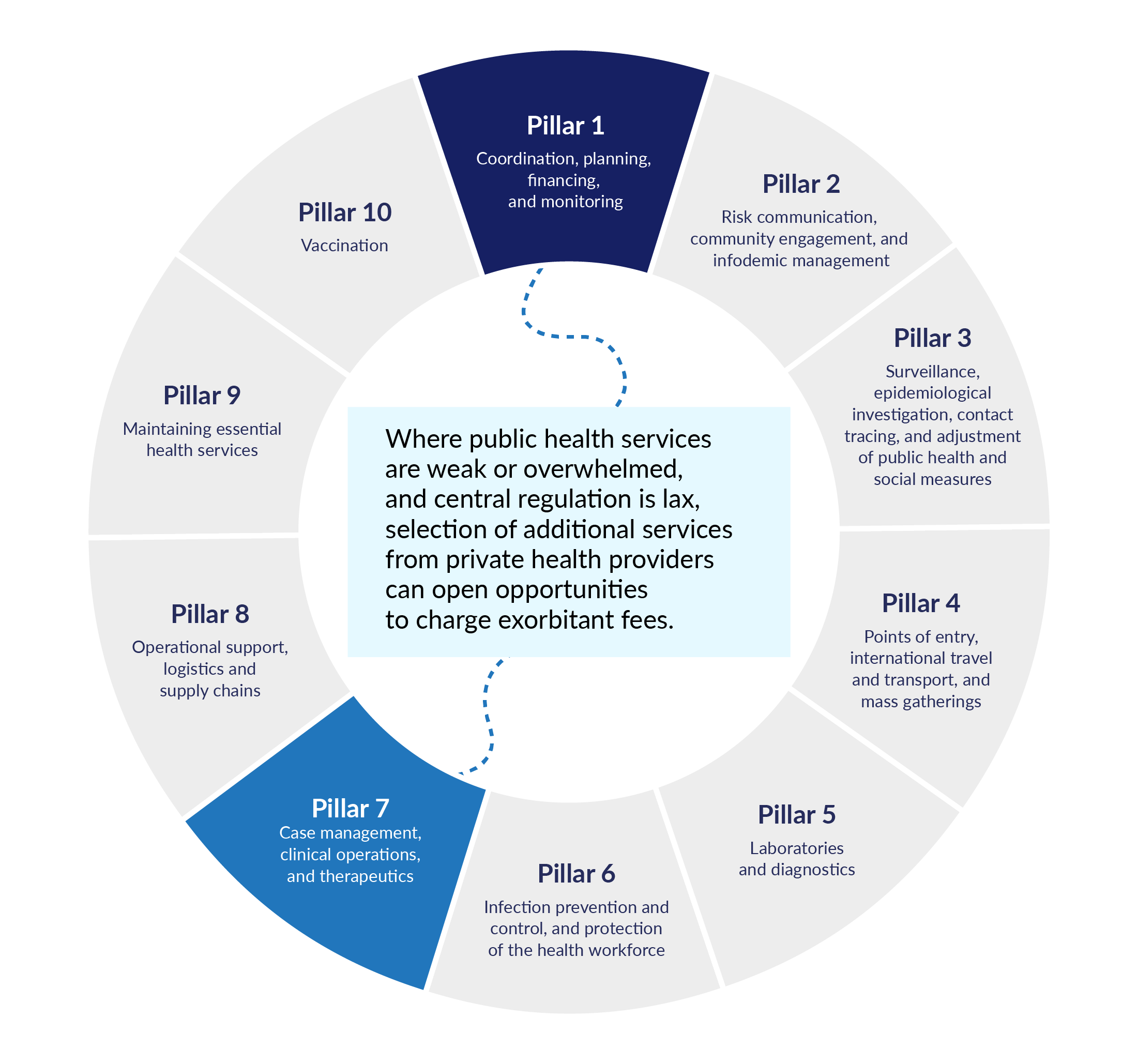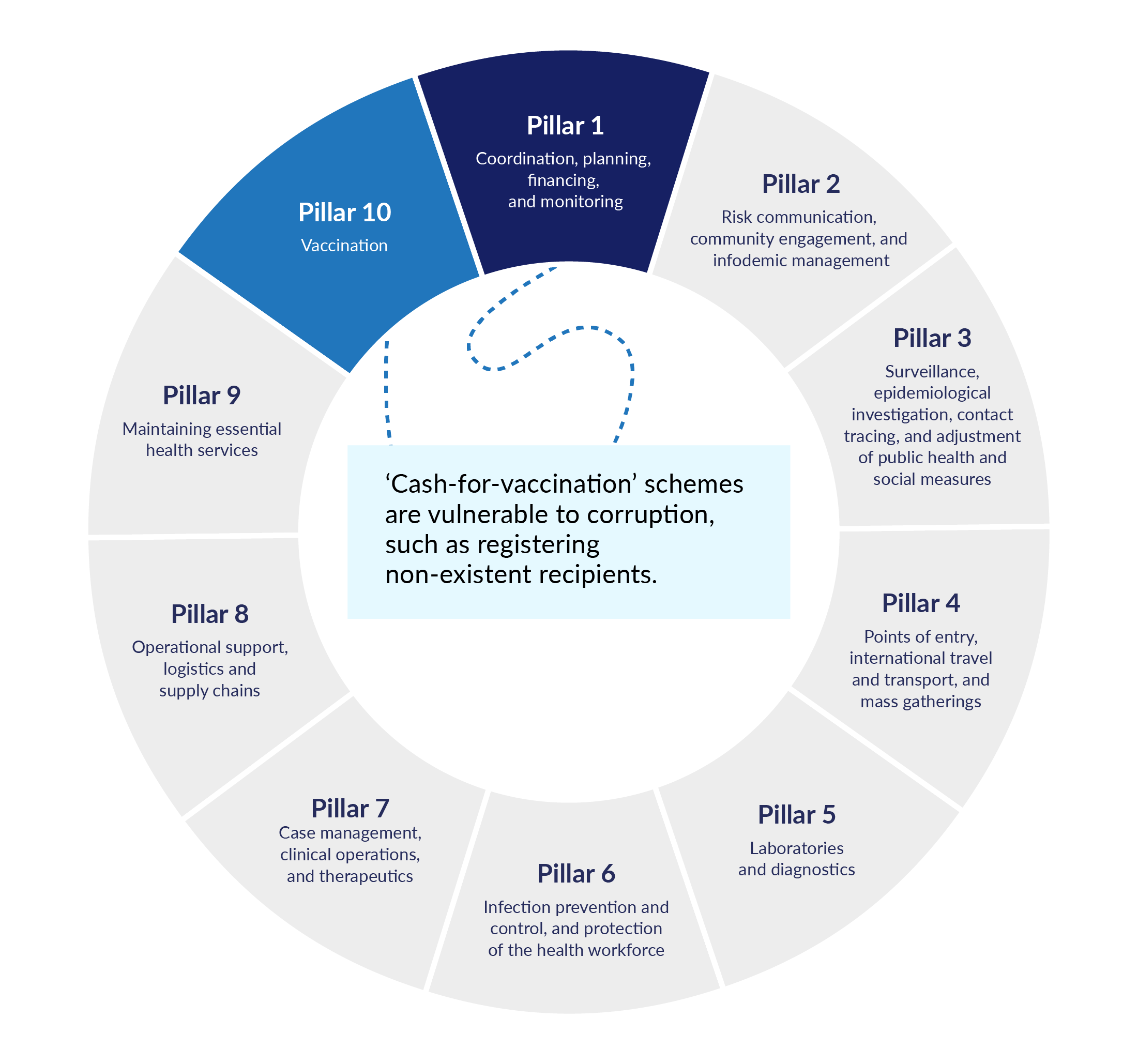
The World Health Organization’s emergency response is managed through its Incident Management System (IMS). This standardized but flexible approach applies regardless of the underlying hazard, scale, or context of the emergency. To assist WHO and Member States to respond, response plans are developed, and for Covid-19 this was set out as ten ‘pillars’ to adapt as appropriate for each country while retaining a common structure.
These pillars interact and affect one another, but they all depend on Pillar 1 (Coordination, planning, financing, and monitoring). This is where managers of an emergency response set the scope and terms of an emergency response. Decisions made at this stage can open the way for fraud and corruption to appear in other pillars. Fraud and corruption damage health and care outcomes for everyone. They prevent authorities from reaching their public health goals, increase public distrust, and undermine vital health messaging.
The lessons from the research, as set out in this blog series, are not only applicable to Covid-19. We hope that the findings can also support those involved in the decision-making processes for responses to other health and humanitarian challenges, so they can identify and address red flags for corruption early on.
A window into Covid-19 corruption – and a toolkit for addressing it
The pillars allow leaders and practitioners to plan and implement every level and stage of a health emergency. The pillars are also a useful framework to identify and categorise different forms of corruption and fraud during health emergencies. They are a useful way to compartmentalise a pandemic response.
By looking at real-world examples of fraud and corruption, and considering the spaces in which these cases could occur, we can make more effective recommendations for finding and addressing them.
The research
Table 2. A checklist of anti-fraud and anti-corruption measures
|
Theme |
Red flag |
Is red flag present? Y/N |
Recommendations, if red flag is present |
|
Lack of transparency |
Are response plans published and regularly updated? Are statistics and government spending data gathered and published regularly? |
|
|
|
Concentration of power |
Is a single individual or small group responsible for more than one decision-making body? |
|
|
|
Conflicts of interest |
Do implementation managers hold a beneficial interest in potential suppliers or contractors, either directly or via their family or associates? |
|
|
|
Physical discrepancies |
Do products have poor-quality packaging, misspellings on labelling, or exaggerated claims of efficacy? Are there discrepancies in size, weight, quality, colour or packaging between specifications and products actually received? |
|
|
|
Procurement irregularities |
Are simplified procedures used without adequate justification or for extended periods? |
|
|
|
Data anomalies |
Are there discrepancies in data collected on the same topic from different sources (eg, hospital admissions figures differ between local and central data)? |
|
|
|
Whistleblower and public complaints |
Have individuals reported that they have been asked to pay unexpected fees, facilitation payments or bribes to obtain health services such as testing, treatment, or vaccination, or to bypass infection control measures such as testing or quarantine? Have healthcare professionals reported that they have not received specific compensation or incentives allocated for pandemic-related work? |
|
|
The other two blogs in this series give specific recommendations for pillars 1 and 8. You can also find more recommendations from the Covid-19 pandemic in this Issue paper, which summarises the trends, drivers and lessons learned for reducing corruption in health emergencies.
Don’t forget the politics!
It is also important to tailor the framework to any specific setting and context. While these pillar principles may be consistent across the world, in reality, any ‘corruption system’ depends on the power relations and the political economy in a specific country. It is important to not only consider the technical aspects of the pillars but also the underlying politics and complexity at play.
Disclaimer
All views in this text are the author(s)’, and may differ from the U4 partner agencies’ policies.
This work is licenced under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International licence (CC BY-NC-ND 4.0)


